The International Association of Healthcare Security and Safety (IAHSS) released new guidance this week to help healthcare officials prepare for and respond to visitor and patient violence in hospitals.
The guidance boils down to five steps hospital officials can take to better prepare their facilities’ for the potential of violence.
Tom Smith, chair of the IAHSS Counsel on Guidelines, says the guideline complements the Joint Commission’s recently released Sentinel Event Alert on preventing workplace violence.
“This guideline could not be timelier,” Smith says. “The content of the IAHSS “Violent Patient / Patient Visitor Management” guideline will add to and support [the Joint Commission’s] most recent Sentinel Event Alert and assist healthcare organizations as they develop proactive policies and practices to address violent and threatening patients and family members”.
5 Steps to Patient Violence Preparedness
A summary of the IAHSS Patient/Visitor Violence Management guidance is included below.
1. Develop an internal plan for hospital officials to identify and manage violent, threatening or other inappropriate behavior. That process may include:
- A system of identifying risks based on specific escalating behavior and well-defined response procedures. An example of such a system using flags is shown below:
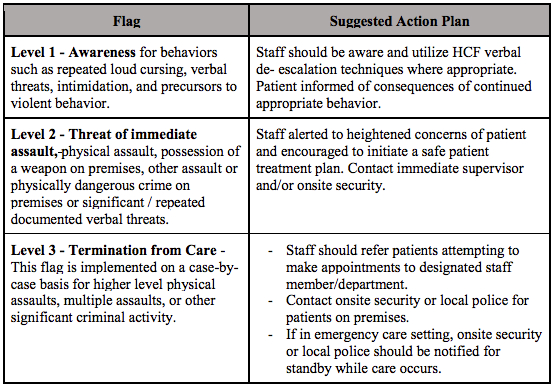
- Using electronic health records (EHR) to flag behavior and gain historical context of a patient and their visitors
- Deciding who in your hospital can initiate a flag
- Establishing behavioral expectations with patients and visitors in the flag system
- Identifying medical factors or other circumstances that may contribute to concerning behaviors
- Establishing a review process to consider removing or downgrading the flag with behavior changes over time
2. Establish criteria for terminating patient care due to violent or inappropriate behavior in accordance with any applicable patient rights and abandonment laws. Hospitals may want to establish a multi-disciplinary team to make those determinations.
3. Change care plans for violent or disruptive patients when terminating care isn’t an option. Risk mitigation options include:
- Changing the treatment room to remove all hazards and unnecessary equipment and furnishings
- Implementing patient search protocols that may include metal screening or removal of patient belongings including clothing; securing and inventorying personal property
- Increasing observation and response capabilities with additional care providers or security officers
- Establishing ways to alert other staff members of the concern, including those without access to the patient’s EHR
- Communicating and reinforcing behavioral expectations with the patient or visitor (this may include discussion with family members)
- Medically-approved patient restraints
4. Develop processes to restrict visitor/patient access to certain or all patients, departments or the entire healthcare facility.
5. Create training programs and attendance expectations with all hospital employees to address the prevention, recognition, avoidance, diffusion, response and reporting of threats, acts of aggression and other behaviors of concern. Education should be appropriate to job function and risk level.
Related IAHSS Guidance
- 01.09 Violence in Healthcare
- 01.09.03 Threat Management Team
- 02.02.04 De-Escalation Training
- 05.02 Security Role in Patient Management
- 05.04 Searching Patients and Patients Areas for Contraband
- 05.06 Security in the Emergency Care Setting